1Department of Laboratory Medicine, National Health Insurance Service Ilsan Hospital, Goyang, 2 Department of Laboratory Medicine, Yonsei University College of Medicine, Seoul, 3Research Institute of Bacterial Resistance, Yonsei University College of Medicine, Seoul, 4Department of Laboratory Medicine, Chonnam National University Medical School, Gwangju, 5Department of Laboratory Medicine, Chungbuk National University College of Medicine, Cheongju, 6Department of Laboratory Medicine and Paik Institute for Clinical Research, Inje University College of Medicine, Busan, 7Department of Laboratory Medicine, Jeju National University College of Medicine, Jeju, 8Department of Laboratory Medicine, Hallym University Dongtan Sacred Heart Hospital, Hallym University College of Medicine, Hwaseong, 9Department of Laboratory Medicine, Yonsei University Wonju College of Medicine, Wonju, 10Department of Laboratory Medicine, Keimyung University School of Medicine, Daegu, Korea
Corresponding to Young Ah Kim, E-mail: yakim@nhimc.or.kr
Ann Clin Microbiol 2022;25(4):137-145. https://doi.org/10.5145/ACM.2022.25.4.4
Received on 16 September 2022, Revised on 15 November 2022, Accepted on 29 November 2022, Published on 20 December 2022.
Copyright © Korean Society of Clinical Microbiology.
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (https://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Background: We compared the antimicrobial resistance rates (AMRs) of major glucose nonfermenting gram-negative bacilli, Acinetobacter baumannii and Pseudomonas aeruginosa, under different clinical conditions. The purpose of the study was to provide useful background data to set up infection control strategies for infection-vulnerable patients.
Methods: The AMRs of blood isolates were compared in various clinical conditions, using data from the Antimicrobial Resistance Surveillance System in Korea.
Results: A. baumannii blood isolates from patients with healthcare-associated infections, inpatients, or intensive care unit (ICU)-admitted patients consistently exhibited higher AMRs to most antimicrobials, except minocycline, tigecycline, and colistin, compared with those from patients with community-acquired infections, outpatients, or non-ICU-admitted patients, respectively. P. aeruginosa blood isolates from patients with healthcare-associated infections showed higher AMRs to most antimicrobials, except ceftazidime and aztreonam, compared with those from patients with community-acquired infections, but not compared to those from inpatients or ICU-admitted patients.
Conclusion: Higher AMRs were associated with A. baumannii bloodstream infections under various clinical conditions, such as healthcare-associated infections and infections in inpatients and ICU-admitted patients. Considering the high AMRs and the limited number of treatment options of A. baumannii, vigorous efforts should be used to prevent the spreading of A. baumannii infections in patients with vulnerable conditions.
Antimicrobial resistance rate, Acinetobacter baumannii, Pseudomonas aeruginosa
Acinetobacter baumannii is a major cause of healthcare-associated infections, resulting in pneumonia, sepsis, endocarditis, urinary tract infection, wound infection, and meningitis, especially in immunocompromised patients [1]. Compared to A. baumannii infections, half of Pseudomonas aeruginosa isolates come from community-acquired infections but also play an important role in healthcare-associated infections [2].
Several factors contribute to outcomes in patients with bacterial infections, including host factors (for example, underlying diseases, demographic conditions), bacteriological factors (for example, virulence factors, antimicrobial susceptibility), and therapeutic modalities (for example, empirical antimicrobial treatment, definitive antimicrobial treatment) [3]. Increasing antimicrobial resistance rates (AMRs) of clinically important glucose non-fermenters such as A. baumannii and P. aeruginosa have become serious problems especially in treating immunocompromised patients.
Our study aims to evaluate the differences of AMRs of A. baumannii or P. aeruginosa blood isolates according to clinical conditions. The purpose of the study is to provide useful background data in setting up infection control strategies for infection vulnerable patients.
Non-duplicated A. baumannii and P. aeruginosa blood isolates were serially collected from nine nationwide general hospitals (National Health Insurance Service Ilsan Hospital, Gangnam Severance Hospital, Chonnam National University Hospital, Chungbuk National University Hospital, Busan Paik Hospital, Jeju National University Hospital, Hallym University Dongtan Sacred Heart Hospital, Wonju Severance Christian Hospital, Keimyung University Dongsan Hospital) in 2021, using the Antimicrobial Resistance Surveillance System in Korea protocols [4]. A. baumannii (n = 229) and P. aeruginosa (n = 233) were included in this study. We verified the bacterial species by using matrix-assisted laser desorption/ ionization time-of-flight mass spectrometry (Bruker Biotyper, Bruker Daltonics GmbH, Bremen, Germany) and confirmed A. baumannii isolates using oxacillinase (OXA)-51 polymerase chain reaction [4].
Antimicrobial susceptibility was mainly determined with the disk diffusion test according to the Clinical and Laboratory Standards Institute guidelines [5]. Colistin susceptibility was tested by the broth microdilution method, a refence method used for colistin testing [6]. The A. baumannii test panel included piperacillin, ampicillin-sulbactam, piperacillin-tazobactam, ceftazidime, cefepime, imipenem, meropenem, amikacin, gentamicin, tobramycin, ciprofloxacin, minocycline, tigecycline, and colistin. The P. aeruginosa test panel included piperacillin, piperacillin-tazobactam, ceftazidime, cefepime, imipenem, meropenem, amikacin, gentamicin, tobramycin, ciprofloxacin, and aztreonam.
We compared clinical conditions, reflecting host clinical conditions such as community-acquired infection/ healthcare-associated infection, intensive care unit (ICU)/non-ICU, and inpatient/outpatient. Communityacquired infection was defined when the specimen was taken either from an outpatient or from a patient hospitalized for less than two calendar days. Healthcare-associated infection was defined when the specimen was taken from a patient hospitalized for two or more calendar days overall, including the hospitalization days in another healthcare facility before transfer. Outpatients also included emergency room patients.
For statistical analysis, we used the Chi-square test and Fisher’s exact test with SAS version 9.4 (SAS Institute, Cary, NC, USA), and categorical variables were expressed in number (%).
The resistance rate of A. baumannii was very high in most antimicrobials except for minocycline, tigecycline, and colistin, whose sensitivity is well preserved (Fig. 1A). The carbapenem resistance rate was as high as approximately 87%. The P. aeruginosa showed less resistant AMRs than that of A. baumannii, with the 37% of imipenem resistance rate (Fig. 1B).
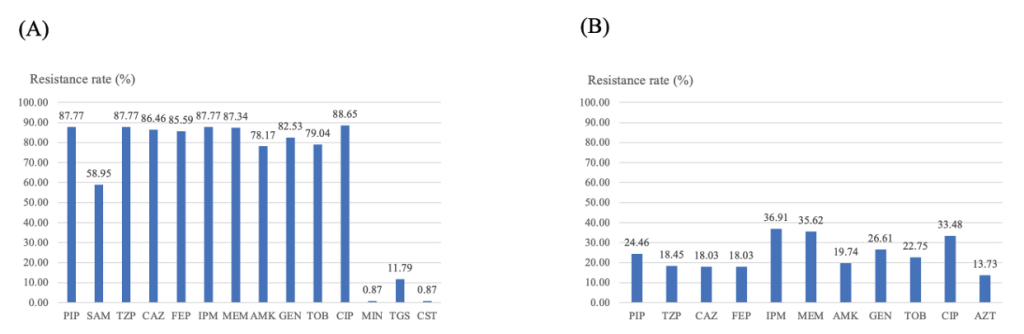
Fig. 1. AMRs of Acinetobacter baumannii (A) and Pseudomonas aeruginosa blood isolates (B). Abbreviations: AMR, antimicrobial resistance rates; PIP, piperacillin; SAM, ampicillin-sulbactam; TZP, piperacillin-tazobactam; CAZ, ceftazidime; FEP, cefepime; IPM, imipenem; MEM, meropenem; AMK, amikacin; GEN, gentamicin; TOB, tobramycin; CIP, ciprofloxacin; MIN, minocycline; TGC, tigecycline; CST, colistin; AZT, aztreonam.
Patients with healthcare-associated infections, inpatients, or ICU-admitted patients consistently exhibited higher AMRs to most antimicrobials except for minocycline, tigecycline, and colistin, compared with that of community-acquired infections, outpatients or non-ICU-admitted patients, respectively (Table 1, Fig. 2).
Patients with healthcare-associated infection showed higher AMRs to most antimicrobials except for ceftazidime and aztreonam, compared with that of community-acquired infections (Table 2). These differences were not prominent in ICU-admitted patients or inpatients, compared to that of non-ICUadmitted patients or outpatients, respectively.
Table 1. Comparison of antimicrobial resistance rates of Acinetobacter baumannii blood isolates in groups
| ANTI | CA (n = 31) | HA (n = 198) | P-value | Non-ICU (n = 97) | ICU (n = 132) | P-value | Inpatient (n = 206) | Outpatient (n = 23) | P-value | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| No. | (%) | No. | (%) | No. | (%) | No. | (%) | No. | (%) | No. | (%) | |||||||
| PIP | < 0.0001 | < 0.0001 | < 0.0001 | |||||||||||||||
| S or I | 13 | (41.94) | 15 | (7.58) | 24 | (24.74) | 4 | (3.03) | 18 | (8.74) | 10 | (43.48) | ||||||
| R | 18 | (58.06) | 183 | (92.42) | 73 | (75.26) | 128 | (96.97) | 188 | (91.26) | 13 | (56.52) | ||||||
| SAM | 0.0932 | 0.0009 | 0.0007 | |||||||||||||||
| S or I | 17 | (54.84) | 77 | (38.89) | 52 | (53.61) | 42 | (31.82) | 77 | (37.38) | 17 | (73.91) | ||||||
| R | 14 | (45.16) | 121 | (61.11) | 45 | (46.39) | 90 | (68.18) | 129 | (62.62) | 6 | (26.09) | ||||||
| TZP | < 0.0001 | < 0.0001 | < 0.0001 | |||||||||||||||
| S or I | 13 | (41.94) | 15 | (7.58) | 24 | (24.74) | 4 | (3.03) | 18 | (8.74) | 10 | (43.48) | ||||||
| R | 18 | (58.06) | 183 | (92.42) | 73 | (75.26) | 128 | (96.97) | 188 | (91.26) | 13 | (56.52) | ||||||
| CAZ | < 0.0001 | < 0.0001 | 0.0002 | |||||||||||||||
| S or I | 13 | (41.94) | 18 | (9.09) | 27 | (27.84) | 4 | (3.03) | 21 | (10.19) | 10 | (43.48) | ||||||
| R | 18 | (58.06) | 180 | (90.91) | 70 | (72.16) | 128 | (96.97) | 185 | (89.81) | 13 | (56.52) | ||||||
| FEP | < 0.0001 | < 0.0001 | < 0.0001 | |||||||||||||||
| S or I | 13 | (41.94) | 20 | (10.10) | 26 | (26.80) | 7 | (5.3) | 22 | (10.68) | 11 | (47.83) | ||||||
| R | 18 | (58.06) | 178 | (89.90) | 71 | (73.20) | 125 | (94.7) | 184 | (89.32) | 12 | (52.17) | ||||||
| IPM | < 0.0001 | < 0.0001 | 0.0004 | |||||||||||||||
| S or I | 12 | (38.71) | 16 | (8.08) | 24 | (24.74) | 4 | (3.03) | 19 | (9.22) | 9 | (39.13) | ||||||
| R | 19 | (61.29) | 182 | (91.92) | 73 | (75.26) | 128 | (96.97) | 187 | (90.78) | 14 | (60.87) | ||||||
| MEM | < 0.0001 | < 0.0001 | < 0.0001 | |||||||||||||||
| S or I | 13 | (41.94) | 16 | (8.08) | 25 | (25.77) | 4 | (3.03) | 19 | (9.22) | 10 | (43.48) | ||||||
| R | 18 | (58.06) | 182 | (91.92) | 72 | (74.23) | 128 | (96.97) | 187 | (90.78) | 13 | (56.52) | ||||||
| AMK | < 0.0001 | < 0.0001 | < 0.0001 | |||||||||||||||
| S or I | 17 | (54.84) | 33 | (16.67) | 39 | (40.21) | 11 | (8.33) | 36 | (17.48) | 14 | (60.87) | ||||||
| R | 14 | (45.16) | 165 | (83.33) | 58 | (59.79) | 121 | (91.67) | 170 | (82.52) | 9 | (39.13) | ||||||
| GEN | < 0.0001 | < 0.0001 | 0.0004 | |||||||||||||||
| S or I | 15 | (48.39) | 25 | (12.63) | 33 | (34.02) | 7 | (5.3) | 29 | (14.08) | 11 | (47.83) | ||||||
| R | 16 | (51.61) | 173 | (87.37) | 64 | (65.98) | 125 | (94.7) | 177 | (85.92) | 12 | (52.17) | ||||||
| TOB | < 0.0001 | < 0.0001 | < 0.0001 | |||||||||||||||
| S or I | 16 | (51.61) | 32 | (16.16) | 39 | (40.21) | 9 | (6.82) | 35 | (16.99) | 13 | (56.52) | ||||||
| R | 15 | (48.39) | 166 | (83.84) | 58 | (59.79) | 123 | (93.18) | 171 | (83.01) | 10 | (43.48) | ||||||
| CIP | < 0.0001 | < 0.0001 | 0.0002 | |||||||||||||||
| S or I | 12 | (38.71) | 14 | (7.07) | 22 | (22.68) | 4 | (3.03) | 17 | (8.25) | 9 | (39.13) | ||||||
| R | 19 | (61.29) | 184 | (92.93) | 75 | (77.32) | 128 | (96.97) | 189 | (91.75) | 14 | (60.87) | ||||||
| MIN | > 0.9999 | > 0.9999 | > 0.9999 | |||||||||||||||
| S or I | 31 | (100.00) | 196 | (98.99) | 96 | (98.97) | 131 | (99.24) | 204 | (99.03) | 23 | (100.00) | ||||||
| R | – | 0 | 2 | (1.01) | 1 | (1.03) | 1 | (0.76) | 2 | (0.97) | – | 0 | ||||||
| TGC | 0.5474 | 0.3123 | 0.3264 | |||||||||||||||
| S or I | 29 | (93.55) | 173 | (87.37) | 88 | (90.72) | 114 | (86.36) | 183 | (88.83) | 19 | (82.61) | ||||||
| R | 2 | (6.45) | 25 | (12.63) | 9 | (9.28) | 18 | (13.64) | 23 | (11.17) | 4 | (17.39) | ||||||
| CST | > 0.9999 | > 0.9999 | > 0.9999 | |||||||||||||||
| S or I | 31 | (100.00) | 196 | (98.99) | 96 | (98.97) | 131 | (99.24) | 204 | (99.03) | 23 | (100.00) | ||||||
| R | – | 0 | 2 | (1.01) | 1 | (1.03) | 1 | (0.76) | 2 | (0.97) | – | 0 | ||||||
Bold form: statistically significant. Abbreviations: ANTI, antimicrobials; CA, community-acquired infection; HA, healthcare-associated infection; ICU, intensive care unit; PIP, piperacillin; SAM, ampicillin-sulbactam; TZP, piperacillin-tazobactam; CAZ, ceftazidime; FEP, cefepime; IPM, imipenem; MEM, meropenem; AMK, amikacin; GEN, gentamicin; TOB, tobramycin; CIP, ciprofloxacin; MIN, minocycline; TGC, tigecycline; CST, colistin; S, susceptible; I, intermediate; R, resistant.
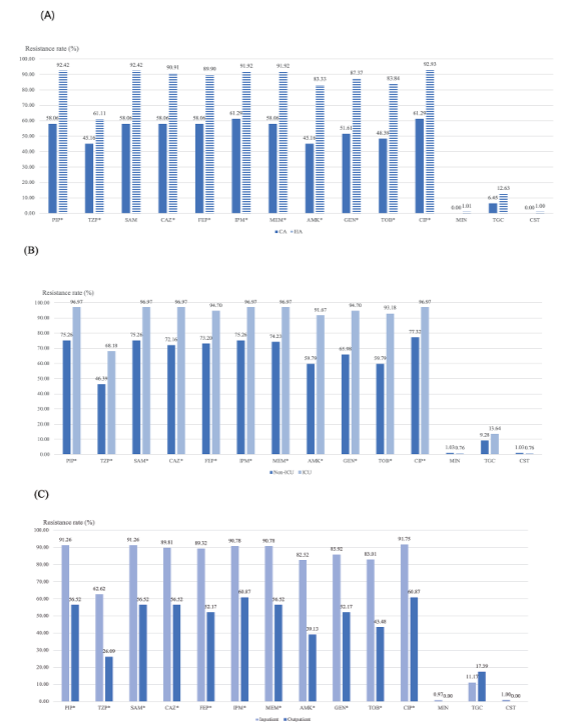
Table 2. Comparison of antimicrobial resistance rates of Pseudomonas aeruginosa blood isolates in groups
| ANTI | CA (n = 100) | HA (n = 133) | P-value | Non-ICU (n = 168) | ICU (n = 65) | P-value | Inpatient (n = 179) | Outpatient (n = 54) | P-value | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| No. | (%) | No. | (%) | No. | (%) | No. | (%) | No. | (%) | No. | (%) | |||||||
| PIP | 0.0092 | 0.4758 | 0.0249 | |||||||||||||||
| S or I | 84 | (84.00) | 92 | (69.17) | 129 | (76.79) | 47 | (72.31) | 129 | (72.07) | 47 | (87.04) | ||||||
| R | 16 | (16.00) | 41 | (30.83) | 39 | (23.21) | 18 | (27.69) | 50 | (27.93) | 7 | (12.96) | ||||||
| TZP | 0.0039 | 0.258 | 0.0469 | |||||||||||||||
| S or I | 90 | (90.00) | 100 | (75.19) | 140 | (83.33) | 50 | (76.92) | 141 | (78.77) | 49 | (90.74) | ||||||
| R | 10 | (10.00) | 33 | (24.81) | 28 | (16.67) | 15 | (23.08) | 38 | (21.23) | 5 | (9.26) | ||||||
| CAZ | 0.1657 | 0.7853 | 0.2695 | |||||||||||||||
| S or I | 86 | (86.00) | 105 | (78.95) | 137 | (81.55) | 54 | (83.08) | 144 | (80.45) | 47 | (87.04) | ||||||
| R | 14 | (14.00) | 28 | (21.05) | 31 | (18.45) | 11 | (16.92) | 35 | (19.55) | 7 | (12.96) | ||||||
| FEP | 0.0156 | 0.5142 | 0.0559 | |||||||||||||||
| S or I | 89 | (89.00) | 102 | (76.69) | 136 | (80.95) | 55 | (84.62) | 142 | (79.33) | 49 | (90.74) | ||||||
| R | 11 | (11.00) | 31 | (23.31) | 32 | (19.05) | 10 | (15.38) | 37 | (20.67) | 5 | (9.26) | ||||||
| IPM | < 0.0001 | 0.0064 | 0.0004 | |||||||||||||||
| S or I | 79 | (79.00) | 68 | (51.13) | 115 | (68.45) | 32 | (49.23) | 102 | (56.98) | 45 | (83.33) | ||||||
| R | 21 | (21.00) | 65 | (48.87) | 53 | (31.55) | 33 | (50.77) | 77 | (43.02) | 9 | (16.67) | ||||||
| MEM | 0.0005 | 0.007 | 0.0432 | |||||||||||||||
| S or I | 77 | (77.00) | 73 | (54.89) | 117 | (69.64) | 33 | (50.77) | 109 | (60.89) | 41 | (75.93) | ||||||
| R | 23 | (23.00) | 60 | (45.11 | 51 | (30.36) | 32 | (49.23) | 70 | (39.11) | 13 | (24.07) | ||||||
| AMK | 0.01 | 0.1262 | 0.1533 | |||||||||||||||
| S or I | 88 | (88.00) | 99 | (74.44) | 139 | (82.74) | 48 | (73.85) | 140 | (78.21) | 47 | (87.04) | ||||||
| R | 12 | (12.00) | 34 | (25.56) | 29 | (17.26) | 17 | (26.15) | 39 | (21.79) | 7 | (12.96) | ||||||
| GEN | 0.004 | 0.12 | 0.0252 | |||||||||||||||
| S or I | 83 | (83.00) | 88 | (66.17) | 128 | (76.19) | 43 | (66.15) | 125 | (69.83) | 46 | (85.19) | ||||||
| R | 17 | (17.00) | 45 | (33.83) | 40 | (23.81) | 22 | (33.85) | 54 | (30.17) | 8 | (14.81) | ||||||
| TOB | 0.0057 | 0.1419 | 0.0504 | |||||||||||||||
| S or I | 86 | (86.00) | 94 | (70.68) | 134 | (79.76) | 46 | (70.77) | 133 | (74.3) | 47 | (87.04) | ||||||
| R | 14 | (14.00) | 39 | (29.32) | 34 | (20.24) | 19 | (29.23) | 46 | (25.7) | 7 | (12.96) | ||||||
| CIP | 0.0033 | 0.1893 | 0.1798 | |||||||||||||||
| S or I | 77 | (77.00) | 78 | (58.65) | 116 | (69.05) | 39 | (60.00) | 115 | (64.25) | 40 | (74.07) | ||||||
| R | 23 | (23.00) | 55 | (41.35) | 52 | (30.95) | 26 | (40.00) | 64 | (35.75) | 14 | (25.93) | ||||||
| ATM | 0.2931 | 0.6940 | 0.1233 | |||||||||||||||
| S or I | 89 | (89.00) | 112 | (84.21) | 144 | (85.71) | 57 | (87.69) | 151 | (84.36) | 50 | (92.59) | ||||||
| R | 11 | (11.00) | 21 | (15.79) | 24 | (14.29) | 8 | (12.31) | 28 | (15.64) | 4 | (7.41) | ||||||
Bold form: statistically significant. Abbreviations: ANTI, antimicrobials; CA, community-acquired infection; HA, healthcare-associated infection; ICU, intensive care unit; PIP, piperacillin; TZP, piperacillin-tazobactam; CAZ, ceftazidime; FEP, cefepime; IPM, imipenem; MEM, meropenem; AMK, amikacin; GEN, gentamicin; TOB, tobramycin; CIP, ciprofloxacin; ATM, aztreonam; S, susceptible; I, intermediate; R, resistant
Carbapenem has been widely used as the treatment of choice for extended-spectrum-β-lactamase Escherichia coli or Klebsiella pneumoniae infections [7]. We have already reported that frequent use of carbapenem is associated with the rapid growth of carbapenem-resistant A. baumannii (CRAB) infections in Korea since 2007 [8]. Carbapenem resistance of clinically important glucose non-fermenters such as A. baumannii and P. aeruginosa has been regarded as an urgent or serious antimicrobial resistance threat [9].
The main resistance mechanism to CRAB is oxacillinase (OXA)-type β-lactamase, and since the mid2000s, it has been reported that most CRAB isolates produce OXA-23 [10]. Unfortunately, most CRAB isolates exhibit multidrug-resistance or even broad drug-resistance because they carry antimicrobial resistance determinants together with aminoglycosides, fluoroquinolones, and tetracyclines [11]. CRAB treatment options are seriously restricted to last-resort agents such as colistin or tigecycline [11]. But declining colistin or tigecycline efficacy have been reported, and this growing resistance is becoming a major concern [12,13]. This study found a resistance rate of 0.87% to colistin and 11.79% to tigecycline. It is necessary to evaluate the resistance mechanism of tigecycline-resistant A. baumannii strains emerging in Korea with the recent introduction of a plasmid-mediated resistance mechanism.
Since VIM-2-producing P. aeruginosa in Korea was reported in 2002 [14], the resistance mechanism of carbapenem-resistant P. aeruginosa (CRPA) is mainly because of metallo-β-lactamase [15]. CRPA also commonly manifests multidrug-resistance [16]. Treatment options are restricted, and combination therapies have been tried [17].
New effective drugs such as ceftolozane-tazobactam, ceftazidime-avibactam, meropenem-vaborbactam, imipenem-relebactam, and cefiderocol have been introduced and for the past 10 years have been safely used in the US and Europe [18]. According to the American Society of Infectious Disease guidelines, these new agents are recommended as primary treatment options for treating multidrug-resistant Gram-negative bacteria [19,20]. However, in Korea, the introduction of these drugs has been delayed or the national health insurance does not cover them [21], so adequate treatment modalities are lacking.
In this study, the isolates of A. baumannii from bloodstream infections showed higher AMRs to most antimicrobials in conditions of healthcare-associated infections, inpatients, or ICU-admissions. Although it is not definitely suggestive of immunocompromised conditions without reviewing underlying diseases, chemotherapy or immune depressing agents, it is important to define vulnerable conditions, considering high AMRs and limitation of treatment options.
This study was approved by Institutional Review Board of the National Health Insurance Service Ilsan Hospital (IRB No. NHIMC 2022-06-010-002).
Jeong Hwan Shin, Young Uh, and Nam Hee Ryoo are currently editorial board members of the Annals of Clinical Microbiology. However, they were not involved in the review process of this article.
This work was funded (2020E540600) by the Research of Korea Disease Control and Prevention Agency.
1. Ibrahim S, Al-Saryi N, Al-Kadmy IMS, Aziz SN. Multidrug-resistant Acinetobacter baumannii as an emerging concern in hospitals. Mol Biol Rep 2021;48:6987-98. 


2. Reynolds D and Kollef M. The Epidemiology and pathogenesis and treatment of Pseudomonas aeruginosa infections: an update. Drugs 2021;81:2117-31. 


3. Centers for Disease Control and Prevention. Understanding the epidemiologic triangle through infectious disease. https://www.cdc.gov › documents › epi_1_triangle [online] (last visited on 31 August 2022).
4. Kim D, Yoon EJ, Hong JS, Choi MH, Kim HS, Kim YR, et al. Major bloodstream infectioncausing bacterial pathogens and their antimicrobial resistance in South Korea, 20172019: phase I report from Kor-GLASS. Front Microbiol 2022;12:799084. 


5. Clinical and Laboratory Standards Institute (CLSI). Performance standards for antimicrobial susceptibility testing; CLSI supplement M100. Wayne; PA: 2020.
6. Matuschek E, Åhman J, Webster C, Kahlmeter G. Antimicrobial susceptibility testing of colistin – evaluation of seven commercial MIC products against standard broth microdilution for Escherichia coli, Klebsiella pneumoniae, Pseudomonas aeruginosa, and Acinetobacter spp. Clin Microbiol Infect 2018;24:865-70. 

7. Peirano G and Pitout JDD. Extended-spectrum β-lactamase-producing Enterobacteriaceae: update on molecular epidemiology and treatment options. Drugs 2019;79:1529-41. 

8. Kim YA, Park YS, Youk T, Lee H, Lee K. Abrupt increase in rate of imipenem resistance in Acinetobacter baumannii complex strains isolated from general hospitals in Korea and correlation with carbapenem administration during 2002-2013. Ann Lab Med 2018;38:179-81. 


9. Centers for Disease Control and Prevention. Antibiotic resistance threats in the United States 2019. https//www.cdc.gov › 2019-ar-threats-report-508 [online] (last visited on 31 August 2022).
10. Lee YS, Kim YR, Kim JY, Park YJ, Song WK, Shin JH, et al. Increasing prevalence of blaOXA23-carrying Acinetobacter baumannii and the emergence of blaOXA-182-carrying Acinetobacter nosocomialis in Korea. Diagn Microbiol Infect Dis 2013;77:160-3. 

11. Doi Y, Murray GL, Peleg AY. Acinetobacter baumannii: evolution of antimicrobial resistancetreatment options. Semin Respir Crit Care Med 2015;36:85-98. 


12. Yoon EJ, Kim HS, Woo H, Choi YJ, Won D, Choi JR, et al. Trajectory of genetic alterations associated with colistin resistance in Acinetobacter baumannii during an in-hospital outbreak of infection. J Antimicrob Chemother 2022;77:69-73. 

13. Hua X, He J, Wang J, Zhang L, Zhang L, Xu Q, et al. Novel tigecycline resistance mechanisms in Acinetobacter baumannii mediated by mutations in adeS, roB and rrf. Emerg Microbes Infect 2021;10:1404-17. 


14. Lee KW, Lim JB, Yum JH, Yong DE, Chong YS, Kim JM, et al. BlaVIM-2 cassette-containing novel integrons in metallo-beta-lactamase-producing Pseudomonas aeruginosa and Pseudomonas putida isolates disseminated in a Korean hospital. Antimicrob Agents Chemother 2002;46:1053-8. 


15. Hong DJ, Bae IK, Jang IH, Jeong SH, Kang HK, Lee K. Epidemiology and characteristics of metallo-β-lactamase-producing Pseudomonas aeruginosa. Infect Chemother 2015;47:81-97. 



16. Kim D and Jeong SH. Current status of multidrug-resistant bacteria. J Korean Med Assoc 2022;65:468-77. 
17. Paulsson M, Granrot A, Ahl J, Tham J, Resman F, Riesbeck K, et al. Antimicrobial combination treatment including ciprofloxacin decreased the mortality rate of Pseudomonas aeruginosa bacteraemia: a retrospective cohort study. Eur J Clin Microbiol Infect Dis 2017;36:1187-96. 


18. Kang CI. Antibiotics for multidrug-resistant gram-negative bacteria. J Korean Med Assoc 2022;65:490-7. 
19. Tamma PD, Aitken SL, Bonomo RA, Mathers AJ, van Duin D, Clancy CJ. Infectious Diseases Society of America guidance on the treatment of AmpC β-lactamase-producing enterobacterales, carbapenem-resistant Acinetobacter baumannii, and Stenotrophomonas maltophilia infections. Clin Infect Dis 2022;74:2089-114. 

20. Tamma PD, Aitken SL, Bonomo RA, Mathers AJ, van Duin D, Clancy CJ. Infectious Diseases Society of America guidance on the treatment of extended-spectrum β-lactamase producing Enterobacterales (ESBL-E), carbapenem-resistant Enterobacterales (CRE), and Pseudomonas aeruginosa with difficult-to-treat resistance (DTR-P. aeruginosa). Clin Infect Dis 2021;72:e169-83. 

21. Lee HJ and Lee DG. Urgent need for novel antibiotics in Republic of Korea to combat multidrug-resistant bacteria. Korean J Intern Med 2022;37:271-80. 



1. Ibrahim S, Al-Saryi N, Al-Kadmy IMS, Aziz SN. Multidrug-resistant Acinetobacter baumannii as an emerging concern in hospitals. Mol Biol Rep 2021;48:6987-98.
2. Reynolds D and Kollef M. The Epidemiology and pathogenesis and treatment of Pseudomonas aeruginosa infections: an update. Drugs 2021;81:2117-31.
3. Centers for Disease Control and Prevention. Understanding the epidemiologic triangle through infectious disease. https://www.cdc.gov › documents › epi_1_triangle [online] (last visited on 31 August 2022).
4. Kim D, Yoon EJ, Hong JS, Choi MH, Kim HS, Kim YR, et al. Major bloodstream infectioncausing bacterial pathogens and their antimicrobial resistance in South Korea, 20172019: phase I report from Kor-GLASS. Front Microbiol 2022;12:799084.
5. Clinical and Laboratory Standards Institute (CLSI). Performance standards for antimicrobial susceptibility testing; CLSI supplement M100. Wayne; PA: 2020.
6. Matuschek E, Åhman J, Webster C, Kahlmeter G. Antimicrobial susceptibility testing of colistin – evaluation of seven commercial MIC products against standard broth microdilution for Escherichia coli, Klebsiella pneumoniae, Pseudomonas aeruginosa, and Acinetobacter spp. Clin Microbiol Infect 2018;24:865-70.
7. Peirano G and Pitout JDD. Extended-spectrum β-lactamase-producing Enterobacteriaceae: update on molecular epidemiology and treatment options. Drugs 2019;79:1529-41.
8. Kim YA, Park YS, Youk T, Lee H, Lee K. Abrupt increase in rate of imipenem resistance in Acinetobacter baumannii complex strains isolated from general hospitals in Korea and correlation with carbapenem administration during 2002-2013. Ann Lab Med 2018;38:179-81.
9. Centers for Disease Control and Prevention. Antibiotic resistance threats in the United States 2019. https//www.cdc.gov › 2019-ar-threats-report-508 [online] (last visited on 31 August 2022).
10. Lee YS, Kim YR, Kim JY, Park YJ, Song WK, Shin JH, et al. Increasing prevalence of blaOXA23-carrying Acinetobacter baumannii and the emergence of blaOXA-182-carrying Acinetobacter nosocomialis in Korea. Diagn Microbiol Infect Dis 2013;77:160-3.
11. Doi Y, Murray GL, Peleg AY. Acinetobacter baumannii: evolution of antimicrobial resistancetreatment options. Semin Respir Crit Care Med 2015;36:85-98.
12. Yoon EJ, Kim HS, Woo H, Choi YJ, Won D, Choi JR, et al. Trajectory of genetic alterations associated with colistin resistance in Acinetobacter baumannii during an in-hospital outbreak of infection. J Antimicrob Chemother 2022;77:69-73.
13. Hua X, He J, Wang J, Zhang L, Zhang L, Xu Q, et al. Novel tigecycline resistance mechanisms in Acinetobacter baumannii mediated by mutations in adeS, roB and rrf. Emerg Microbes Infect 2021;10:1404-17.
14. Lee KW, Lim JB, Yum JH, Yong DE, Chong YS, Kim JM, et al. BlaVIM-2 cassette-containing novel integrons in metallo-beta-lactamase-producing Pseudomonas aeruginosa and Pseudomonas putida isolates disseminated in a Korean hospital. Antimicrob Agents Chemother 2002;46:1053-8.
15. Hong DJ, Bae IK, Jang IH, Jeong SH, Kang HK, Lee K. Epidemiology and characteristics of metallo-β-lactamase-producing Pseudomonas aeruginosa. Infect Chemother 2015;47:81-97.
16. Kim D and Jeong SH. Current status of multidrug-resistant bacteria. J Korean Med Assoc 2022;65:468-77.
17. Paulsson M, Granrot A, Ahl J, Tham J, Resman F, Riesbeck K, et al. Antimicrobial combination treatment including ciprofloxacin decreased the mortality rate of Pseudomonas aeruginosa bacteraemia: a retrospective cohort study. Eur J Clin Microbiol Infect Dis 2017;36:1187-96.
18. Kang CI. Antibiotics for multidrug-resistant gram-negative bacteria. J Korean Med Assoc 2022;65:490-7.
19. Tamma PD, Aitken SL, Bonomo RA, Mathers AJ, van Duin D, Clancy CJ. Infectious Diseases Society of America guidance on the treatment of AmpC β-lactamase-producing enterobacterales, carbapenem-resistant Acinetobacter baumannii, and Stenotrophomonas maltophilia infections. Clin Infect Dis 2022;74:2089-114.
20. Tamma PD, Aitken SL, Bonomo RA, Mathers AJ, van Duin D, Clancy CJ. Infectious Diseases Society of America guidance on the treatment of extended-spectrum β-lactamase producing Enterobacterales (ESBL-E), carbapenem-resistant Enterobacterales (CRE), and Pseudomonas aeruginosa with difficult-to-treat resistance (DTR-P. aeruginosa). Clin Infect Dis 2021;72:e169-83.
21. Lee HJ and Lee DG. Urgent need for novel antibiotics in Republic of Korea to combat multidrug-resistant bacteria. Korean J Intern Med 2022;37:271-80.